Do Herniated Discs Heal on Their Own? What Most People Don’t Realize
It’s one of the most common questions I hear from patients sitting across from me for the first time: “Do herniated discs heal on their own or do I actually need to do something about this?”
The honest answer is more nuanced than a simple yes or no. And because so many people make decisions about their care or their decision not to seek care – based on incomplete information, it’s worth getting this right.
Here’s what the research says, what we see in clinical practice, and what it actually means for your recovery.
Do Herniated Discs Heal on Their Own?
The Short Answer
In some cases – yes, partially. In many cases – not completely.
This distinction matters more than most people realize. Pain may fade. Function may return. But those improvements don’t always mean the disc has fully healed structurally. And assuming recovery because pain has settled is one of the most common reasons we see patients return months later with worsening symptoms.
What “Healing” Actually Means
Pain relief and full recovery are not the same thing. A disc that stops hurting may still remain structurally compromised – with reduced height, altered mechanics, or ongoing nerve proximity that hasn’t resolved. The pain signal quieted; the underlying issue didn’t necessarily go away.
This is an important reframe. Feeling better is progress – but it’s not always the finish line.
How the Body Attempts to Heal a Herniated Disc
The body is genuinely capable of responding to disc injury. Understanding this process helps set realistic expectations.
Natural Inflammatory Response
After a disc herniation, the body triggers an inflammatory response – directing immune cells to the injury site. Over weeks to months, inflammation typically decreases, which is why many people experience gradual pain reduction in the early phase without any formal treatment.
Reabsorption of Disc Material
In some cases, the herniated disc material is actually absorbed by the body over time. A review by Dr. Masui et al., published in Spine Journal, found that larger herniations were more likely to undergo spontaneous reabsorption than smaller contained herniations – a counterintuitive finding that highlights how variable the natural course can be.
Stabilization of the Affected Area
As the body compensates, surrounding muscles and soft tissues tighten around the injured segment to limit movement and protect the area. This stabilization can reduce acute pain – but it also creates postural compensation patterns that often contribute to new problems down the line.
How Long Does Herniated Disc Recovery Take?
Herniated disc recovery time varies considerably based on severity, location, and how well the underlying condition is managed.
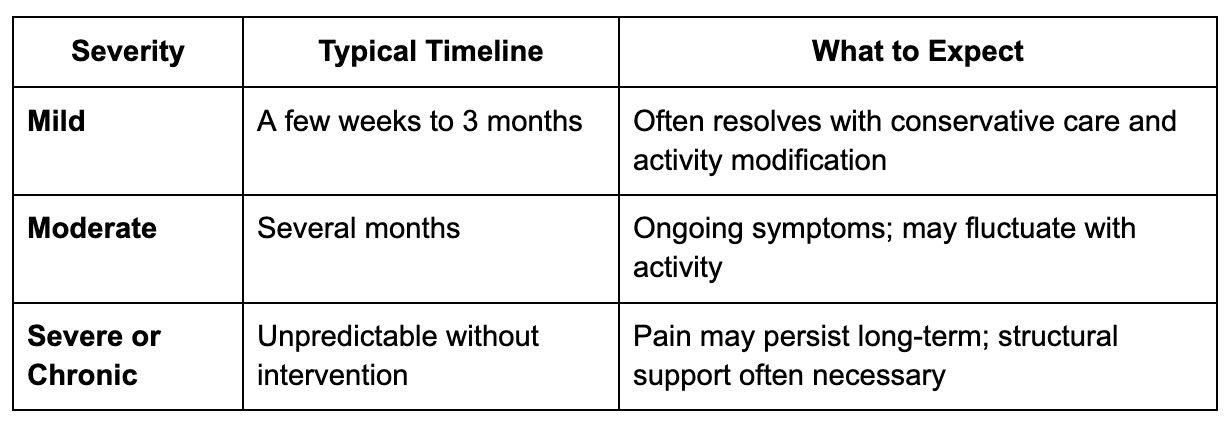
These are general patterns – not guarantees. And the difference between a mild and moderate case can shift quickly without proper management.
Why Some Herniated Discs Do Not Heal on Their Own
Not every disc has a smooth recovery arc. Several factors can interrupt or prevent natural healing entirely.
Continuous Spinal Compression
If the spine remains under constant compressive load – from sitting, poor posture, or occupation – the disc doesn’t get the pressure relief it needs to recover. Think of trying to let a sponge re-expand while someone’s hand is still pressing down on it.
Poor Posture and Lifestyle Habits
Prolonged sitting, forward head posture, and repetitive bending or lifting all sustain the same mechanical stress that caused the injury. Without changing these patterns, healing stalls – regardless of how much rest or medication is involved.
Relying Only on Rest or Medication
Passive management has limits. Rest reduces activity-related aggravation. Medication quiets the pain signal. Neither addresses the disc’s structural environment. Over time, without targeted intervention, the disc can continue to degenerate even when symptoms seem manageable.
Signs Your Herniated Disc Is Not Improving
If you’re monitoring your symptoms and wondering whether to seek care, watch for these indicators that natural recovery may not be on track:
- Pain lasting longer than 3 months – the threshold that defines chronic herniated disc pain
- Radiating pain down the leg – classic sciatica, pointing to nerve compression
- Numbness or tingling in the foot, leg, arm, or hand
- Muscle weakness – difficulty with grip, walking, or weight-bearing
- Increasing difficulty with daily activities – sitting, standing, sleeping, or bending
Any one of these signals warrants evaluation. Together, they strongly suggest the disc is not resolving without support.
Non-Surgical Treatment Options for Herniated Discs
The good news: a herniated disc can often be managed without surgery – especially with early, structured intervention. Here’s how the non-surgical landscape looks:
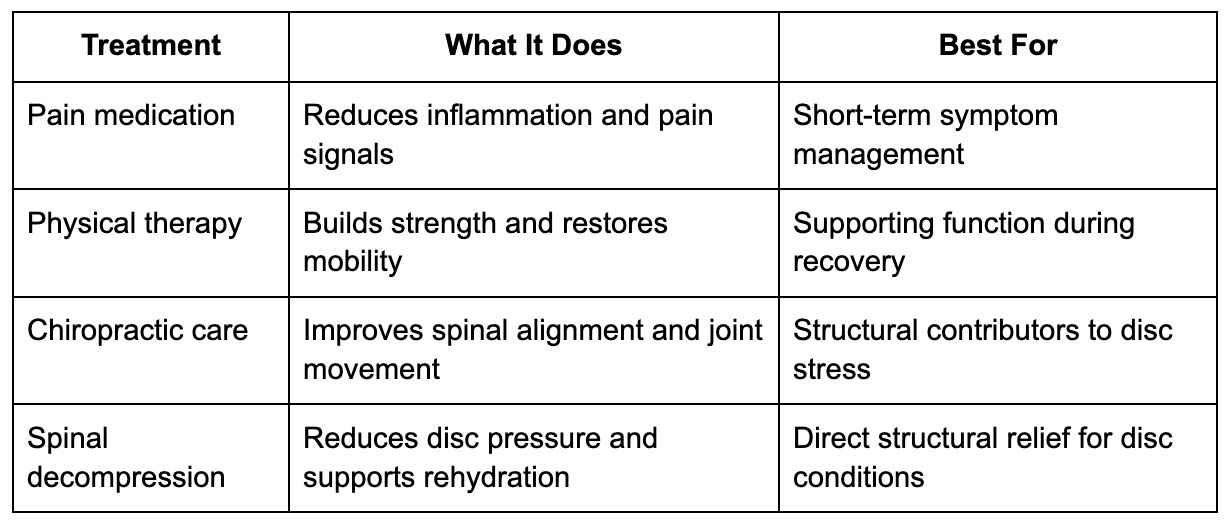
Each of these has a role. The most effective care plans we build use several of these together – not one in isolation.
How Spinal Decompression Therapy Supports Recovery
Of all the non-surgical options, spinal decompression therapy is one of the most directly targeted for disc conditions and it remains one of the most underutilized.
Reducing Pressure on Discs and Nerves
Controlled traction gently separates the vertebrae, creating negative intradiscal pressure. This draws the herniated material away from the nerve – directly addressing the compression that drives pain and dysfunction.
Improving Circulation and Nutrient Exchange
Discs don’t have their own blood supply – they rely on diffusion. Compression blocks this exchange. Decompression restores it, giving the disc the oxygen and nutrients it needs to actually repair.
Supporting Natural Disc Rehydration
A well-hydrated disc is a more resilient disc. Research by Dr. Ralf Benditz, published in the Journal of Back and Musculoskeletal Rehabilitation, found measurable improvements in disc hydration markers following structured decompression therapy – supporting the idea that the therapy enhances, rather than replaces, the body’s natural recovery process.
Final Thoughts: Should You Wait or Take Action?
Some herniated discs do improve naturally. That’s real, and it’s worth acknowledging. But many don’t and the patients who wait the longest often face the longest road to recovery.
The variables that matter most: how severe the herniation is, how long it’s been present, and whether the daily mechanical environment is supporting or undermining healing. None of those can be assessed without a proper evaluation.
Take the Next Step Toward Understanding Your Condition
You don’t have to commit to a treatment plan to get clarity. A proper evaluation tells you what you’re actually dealing with and that knowledge alone changes how you make decisions about your health.
At Newport Center Family Chiropractic, Dr. Mike Digrado brings years of clinical experience in spinal decompression and complex disc conditions to every evaluation. As your trusted Chiropractor Newport Beach, we offer a comprehensive spinal assessment to identify the root cause of your pain and outline the most appropriate path forward – surgical or not.
This article is educational and does not replace a personalized medical evaluation.
See more: How to Prevent a Herniated Disc: Expert Spine Protection Strategies Backed by Science
Newport Center
Family Chiropractic
359 San Miguel Drive
Suite #203
Newport Beach, CA 92660
| Monday | 9:00 AM - 5:00 PM |
| Tuesday | 9:00 AM - 5:00 PM |
| Wednesday | 9:00 AM - 5:00 PM |
| Thursday | 9:00 AM - 5:00 PM |
| Friday | 9:00 AM - 5:00 PM |
| Saturday | 9:00 AM - 12:00 PM |
| Sunday | Closed |
